Do You Need Ultrasound-Guided Joint Injections?
Do you need ultrasound-guided joint injections? Learn when it helps, when it doesn’t, and what really affects your outcome.
Dr. Peter Weil (GP), Claire Weil (RN)
3 min read
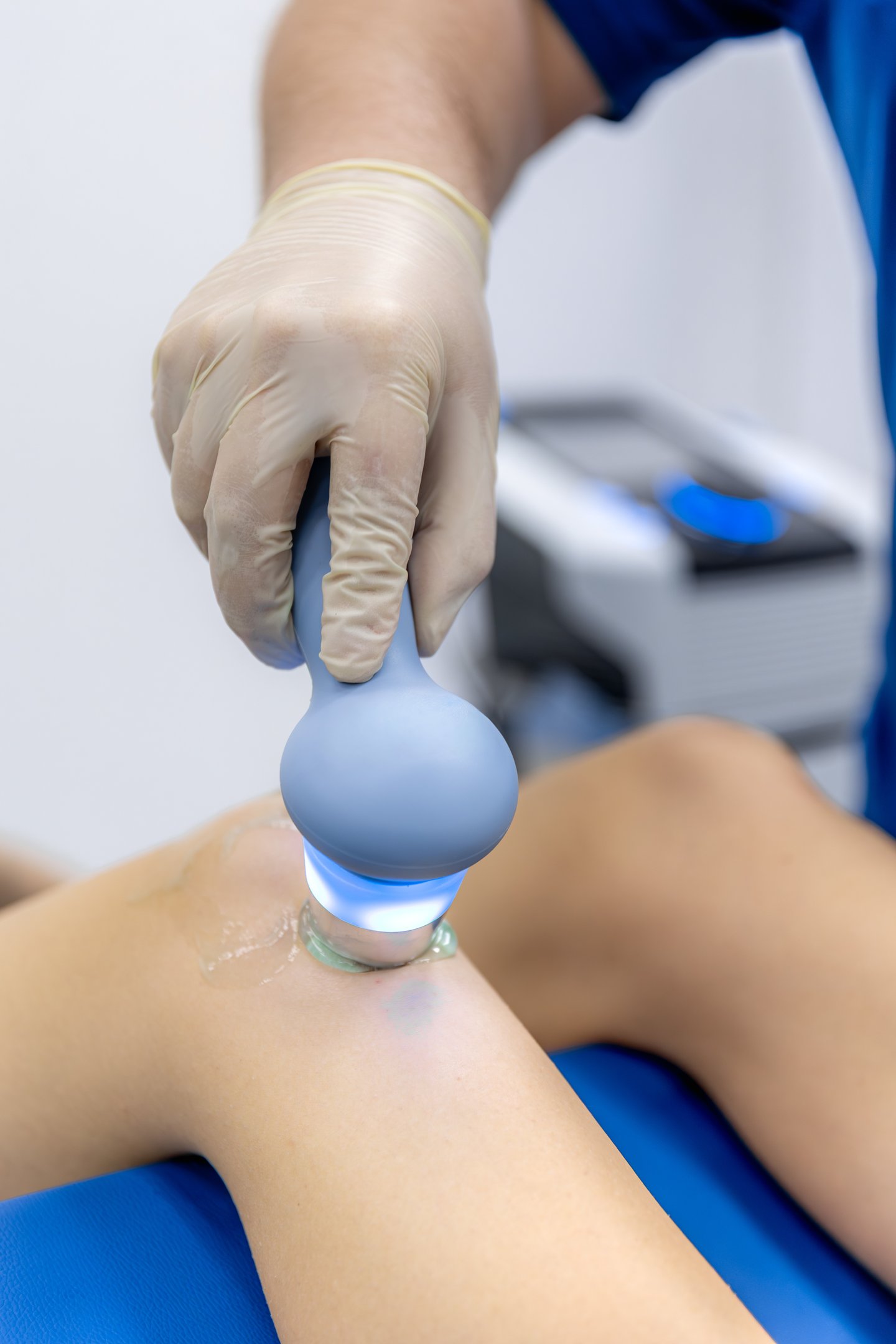
Many patients ask whether ultrasound guidance makes joint injections more effective.
It's a reasonable question. Ultrasound is often described as a more advanced or accurate way of delivering injections, and some clinics promote it as the gold standard.
But the reality is a little more nuanced — and the research evidence may come as a surprise to you.
What does ultrasound guidance actually do?
Ultrasound allows the clinician to see the needle in real time as it enters the joint or soft tissue. This can improve the accuracy of needle placement, help avoid nearby structures such as blood vessels or nerves, and be particularly useful in smaller or more anatomically complex areas.
In certain situations, this can be very helpful.
Does better accuracy mean better results?
Not necessarily.
This is the key point that often gets lost. While ultrasound can improve where the needle goes anatomically, a number of high-quality studies have examined whether this translates into better outcomes for patients — and the picture is more complicated than the technology's reputation might suggest.
A Cochrane systematic review examining ultrasound-guided versus landmark-guided glucocorticoid injections for shoulder pain found no significant difference between the groups in pain or function at one to two weeks or at six weeks when only the highest-quality trials were analysed (Bloom et al., 2012, Cochrane Database of Systematic Reviews. doi:10.1002/14651858.CD009147.pub2).
A more recent systematic review of randomised controlled trials comparing the two approaches for rotator cuff related shoulder pain found that both groups showed significant improvement, with no significant differences between them in pain, function, or range of motion (Adamson et al., 2022, Musculoskeletal Care. doi:10.1002/msc.1643).
A randomised controlled trial of subacromial injections for rotator cuff syndrome found that although ultrasound-guided injections achieved higher anatomical accuracy, there was no meaningful difference in clinical outcomes — pain scores and functional scores improved equally in both groups — leading the authors to conclude that ultrasound guidance was not justified given the comparable efficacy and greater cost of landmark-guided technique (Bhayana et al., 2018, Journal of Clinical Orthopaedics and Trauma. doi:10.1016/j.jcot.2017.01.005).
It is worth noting that the evidence is not entirely one-directional.
Some meta-analyses have found short-term advantages for ultrasound in specific situations, and a major 2025 guideline from multiple American pain medicine societies acknowledges that ultrasound guidance increases injection accuracy and may reduce procedural pain (Benzon et al., 2025, Regional Anesthesia and Pain Medicine. doi:10.1136/rapm-2024-105656). The clinical picture is therefore nuanced, and the value of ultrasound guidance depends on the specific joint, the clinical context, and the experience of the clinician.
When is ultrasound more useful?
There are situations where ultrasound guidance is more likely to make a meaningful difference. These include injections into more complex anatomical targets, cases where anatomy is significantly altered, or where a previous injection has not worked as expected and the precision of delivery needs to be verified.
In these circumstances, ultrasound can help ensure the injection reaches exactly the intended area.
The most important factor
The most important factor in a successful injection is not the technology used. It is accurate diagnosis, appropriate patient selection, skilled technique, and correct aftercare. These are the things that make the biggest difference to outcomes — and they remain constant regardless of the guidance method used.
Our approach
Our focus is always on achieving the best outcome for you.
For the common joint and tendon conditions we treat, landmark-guided injection — performed on the basis of careful clinical examination — is safe, effective, and well supported by evidence. Most patients do very well with this approach.
Where the clinical picture suggests that a different technique is likely to offer a clear benefit, we will always discuss this with you openly.
If you're unsure
If you're unsure whether an injection is right for you, or what approach would be best for your condition, then get in touch. We will always explain our reasoning and answer any questions you have before proceeding.
To learn more about the conditions we treat and how steroid injections may help, visit our Pain By Body Area page. If you're ready to move forward, you can book an appointment.
© Dr. Peter Weil, GP, 2024-2026
Icons and Stock Photos by Freepik and LordIcon
Privacy and GDPR Policy | Terms and Conditions for Website Use & Cookies
ICO registration - ZB780390
The Edinburgh Joint Injection Clinic
@ The Blackford Clinic
60 Blackford Avenue, Edinburgh
07881 902 671
doc@drpeterweil.co.uk
GP-led care with over 15 years' experience in joint injections - clear advice and no pressure to proceed.
